
Serving residents who receive waivered services can enhance both resident outcomes and organizational sustainability, but only when done correctly. Facilities that are unprepared often experience compliance issues, documentation gaps, staff confusion, and financial risk. In contrast, facilities that serve waiver residents well create strong, person-centered environments, maintain regulatory compliance, and optimize reimbursement while supporting residents in living with dignity and choice.
Successfully serving waiver residents requires planning, operational alignment, staff education, and ongoing oversight. Below are key considerations and best practices to help assisted living providers build a sustainable waiver program.
Before accepting waiver residents, facilities must evaluate whether their operations align with HCBS (Home and Community-Based Services) settings requirements in addition to state-assisted living laws.
Key readiness questions include:
Residents must have access to privacy, control over personal space, and access to food and beverages at all times.
Resident must have the freedom to come and go, choose when to wake, eat, or receive services, and have visitors at times of their choosing. Rigid schedules that prioritize operational convenience over resident choice often create compliance concerns.
Policies written for traditional assisted living models may unintentionally restrict waiver residents’ rights. Facilities should review policies related to supervision, safety, behavior management, and daily routines to ensure they support person-centered care.
If gaps are identified, operational changes may be necessary to remain compliant while serving waiver recipients.
Waiver residents require an individualized approach; there is no one-size-fits-all model.
Best practices include:
This individualized approach is a core expectation of waiver services and HCBS compliance.
Waiver residents have separate revenue and distinct revenue streams, which must be clearly understood by leadership, billing staff, and clinical teams:
Facilities must track and manage each independently to ensure accuracy. Confusion between these two payment sources is one of the most common causes of billing errors, recoupments, and audit findings.
Clear internal systems should identify:
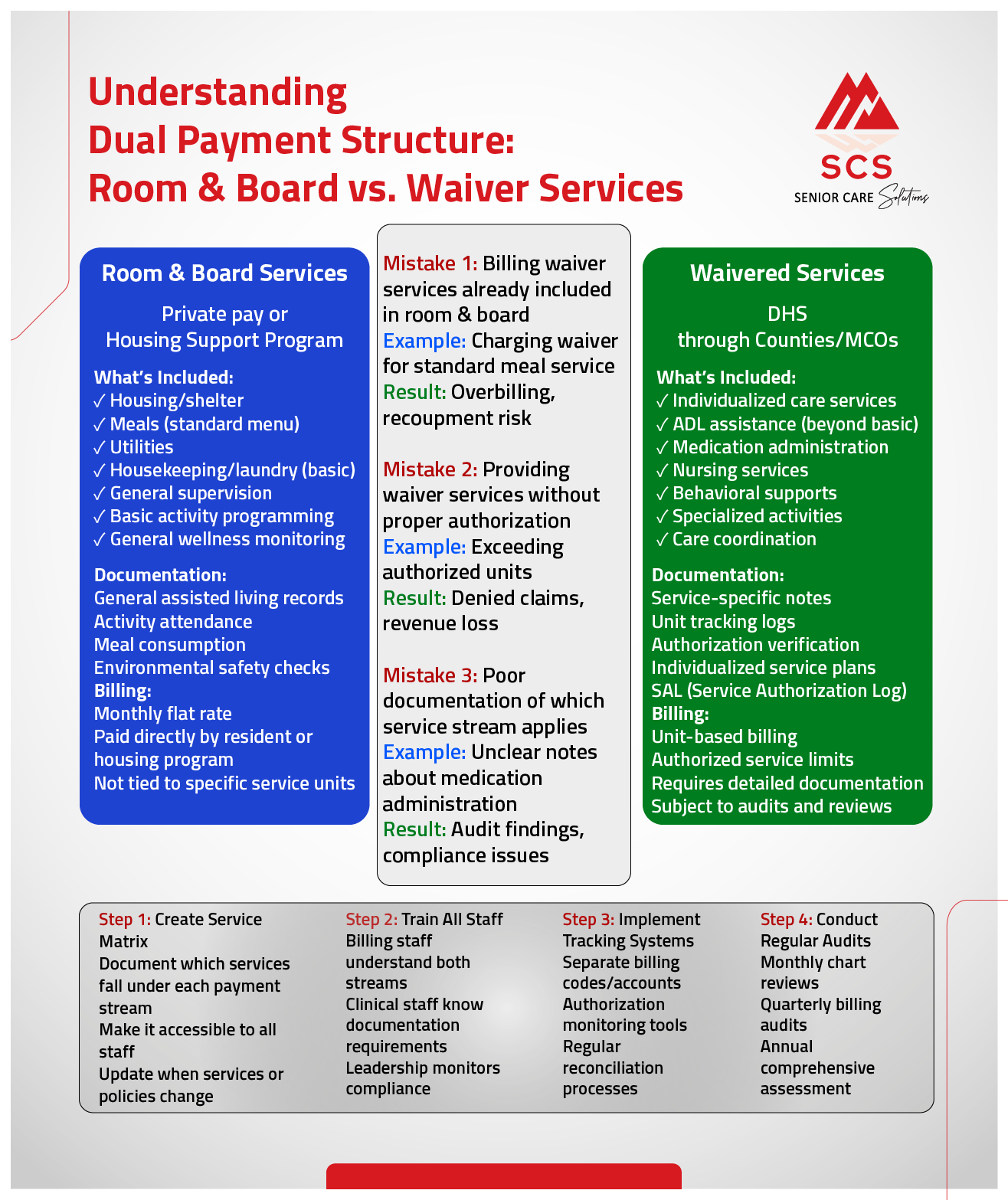
Waiver services are authorized for a specific number of units based on assessed need. Facilities must actively manage these authorizations.
Facilities should:
Failure to manage authorizations can result in denied claims or recoupments.
Strong coordination with external case managers is critical to successful waiver service delivery. Case managers play a key role in authorizations, care planning, and oversight, but they often manage large caseloads and rely on timely, accurate information from facilities.
Facilities should:
Clear and consistent communication prevents service gaps, billing errors, and misunderstandings that can lead to compliance concerns.
Solutions include:
Solutions include:
Solutions include:
Waivered services represent a significant opportunity for assisted living providers to expand their resident base, serve individuals with more complex needs, and fulfill the promise of community-based long-term care. However, successfully participating in waiver programs requires understanding unique requirements, planning, strong clinical oversight, staff education, and ongoing monitoring. When done correctly, it benefits residents, strengthens compliance, and supports financial sustainability.
Whether you're considering accepting your first waiver resident or seeking to improve existing waiver services, our team can provide the guidance and support you need for successful waiver program participation. Contact us today to discuss how waivered services can benefit your assisted living community and your residents.

























